Even with Medicare coverage, medication treatments for hepatitis C can still be costly. According to a 2017 analysis, the cost could range from $6,297 to $10,889 for the entire treatment course. Depending on your income, you may be able to qualify for a low-income subsidy. This means you’d get assistance to pay for your medication costs.
Full Answer
Will insurance pay for HCV treatment?
Nov 18, 2020 · Quotes should be provided by your healthcare provider, commercial insurance provider, Medicaid, Medicare, VA, or other applicable healthcare providers/insurers: 1,2. Mavyret (glecaprevir/pibrentasvir) typically costs $39,600 for a 12-week treatment. Harvoni (ledipasvir/sofosbuvir) typically costs $94,500 for a 12-week treatment.
How much does hepatitis C treatment cost?
High-Cost HCV Drugs in Medicaid: Final Report . 2 . Background . A Brief Epidemiology of Hepatitis C . Hepatitis C is a liver infection caused by the blood-borne hepatitis C virus (HCV), with seven distinct genotypes. 6,7. Transmission occurs mostly by percutaneous exposure, such as unsafe injection practices, needle-
Are there any hepatitis C drugs that are covered by Medicaid?
Update on Medicaid Hepatitis C Virus Drug Coverage John M. Coster, Ph.D., R.Ph. ... • Medicaid controls drug costs primarily through the Federal Medicaid Drug Rebate (MDR) Program and supplemental ... • Indicate Availability of Treatment Guidelines • Restate Rules Regarding MCO Drug Coverage 9.
What are the largest drug costs for Medicare and Medicaid last year?
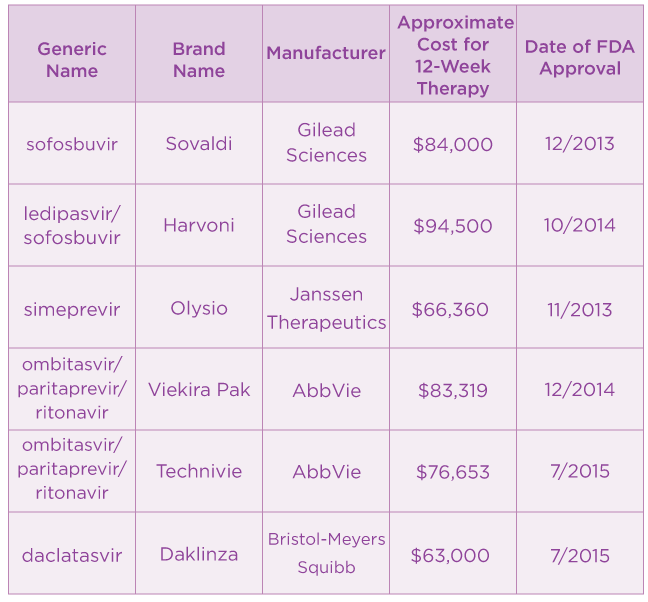
Jun 01, 2018 · The table below highlights the average cost of treatment for the combination DAAs currently available. Most of these drugs take at least 12 weeks to cure HCV, while the most recently approved drug ...

Does insurance cover Hep C drugs?
Not all health insurance plans cover all prescribed medications for HCV treatment with few exceptions. Most insurers cover Sovaldi. It has an estimated copay of $75 to $175 per month. Check with your insurance provider to see what your individual coverage may entail.
How can I get Hep C treatment for free?
Patient assistance programs (PAPs) offer free hepatitis C drugs to lower-income people who are uninsured or underinsured, and who do not qualify for insurance programs such as Medicaid or Medicare.
How do you pay for Hep C treatment?
Funding Resources Available to Hep C PatientsPharmaceutical Programs. ... The American Liver Foundation (ALF) ... NeedyMeds. ... Help-4-Hep. ... The HealthWell Foundation. ... The Pharmaceutical Research and Manufacturers of America (PhRMA) ... The Patient Access Network (PAN) Foundation. ... The Patient Advocate Foundation.Jun 9, 2021
How much does it cost to get rid of Hep C?
The Cost of Hepatitis C Treatment Harvoni cost even more -- $94,500 for a 12-week course, though some patients may be cured after only eight weeks, or $63,000. Gilead's newer offering, Epclusa, goes for just over $74,000. The gamechanger in the market may be Mavyret, which costs $26,500 for treatment.Sep 30, 2019
Does Medicaid cover hep C treatment?
Although it is expensive, there are resources to help you pay for your hep C treatment. Medicaid and most insurance companies cover it.
Will you always test positive for hep C?
A reactive or positive antibody test means you have been infected with the hepatitis C virus at some point in time. Once people have been infected, they will always have antibodies in their blood. This is true if they have cleared the virus, have been cured, or still have the virus in their blood.
How long do you have to be clean to get hep C treatment?
Researchers studied Medicaid programs in the United States from 2017 to 2020. They found that many states require a 6-month to 1-year period of sobriety before someone can start HCV treatment.Dec 16, 2020
What drug cures hep C?
Hepatitis C is treated using direct-acting antiviral (DAA) tablets. DAA tablets are the safest and most effective medicines for treating hepatitis C. They're highly effective at clearing the infection in more than 90% of people. The tablets are taken for 8 to 12 weeks.
Can hep C go away on it's own?
Hepatitis C is a serious liver infection caused by the hepatitis C virus. It is spread from person to person through contact with blood. Most people who are infected with hepatitis C don't experience any symptoms for years. However, hepatitis C usually is a chronic illness (which means it doesn't go away on its own).Jun 4, 2020
Is hep C curable 2020?
Hepatitis C (hep C) infection used to be a lifelong condition for most people. Up to 50 percent of people may clear the hepatitis C virus (HCV) from their body without treatment. For everyone else, the infection becomes chronic. With advances in hep C treatment, most people can now be cured of HCV.
What are the side effects of hep C treatment?
You can expect to have:Flu-like side effects (fever, headache, chills, muscle aches)Gastrointestinal problems (low appetite, nausea, vomiting, diarrhea)Low blood cell counts.Depression.Insomnia.Hair loss.Apr 25, 2021
What is the primary concern that state officials and managed care plans raised about the new HCV drugs?
Respondents in all states agreed that the budget impact from the new HCV medications is substantial, and no state could afford to treat every infected beneficiary in a short period of time . As in the case of prior authorization, states used a range of approaches to try to manage the overall costs of HCV drugs.
What are the challenges of HCV?
States used a variety of approaches to help plans cover the costs of HCV medications, but they fall into roughly three categories: (1) supplemental or “kick” payments; (2) risk sharing; and (3) carve out – that is, direct state management and payment for HCV medications.
How many genotypes of hepatitis C are there?
Hepatitis C is a liver infection caused by the blood-borne hepatitis C virus (HCV), with seven distinct genotypes.6,7 Transmission occurs mostly by percutaneous exposure, such as unsafe injection practices, needle-stick injury, or inadequate infection control. Infection may be acute or chronic. Acute infections are not life-threatening and often clear in less than a year without treatment. However, most people who are infected (55% to 85%) develop chronic HCV infections, and 15% to 30% of these people develop liver cirrhosis within 20 years.8
Does AASLD encourage substance use?
Respondents in several states noted that AASLD/IDSA guidelines now encourage treatment of patients with a substance use disorder (SUD), past or active. One state official also remarked that their discussions with representatives of the VA suggested that rates of adherence and successful treatment among patients with SUD were “quite good” with proper clinical support. These factors influence decisions to curtail substance use restrictions on access to treatment, although many states continue to consider substance use in prior authorization protocols.
How to pay for HCV?
If you’re concerned about paying for HCV medications, remember that you aren’t alone as you seek treatment. There are people and organizations that can help you, including the following: 1 Your doctor. They can help you by ordering and documenting the tests you’ll need so you can qualify to get your medications, especially if you’re working with a liver or infection specialist. 2 Most drug manufacturers. There are patient assistance programs that offer free or reduced-cost medications for people who meet their criteria. 3 Patient advocacy groups. These groups provide assistance with all aspects of HCV treatment. For instance, if your insurer denies treatment, you can appeal the decision with help from one of these groups. Your doctor can also help in this situation.
How many people die from hepatitis C each year?
Americans have chronic hepatitis C. About 19,000 of these people die each year from cirrhosis or liver cancer. Fortunately, recent advancements in the fight against this virus have changed the outlook for people with HCV. New drugs have transformed the disease from one that can, at best, be controlled to one that can be cured for most people who ...
What is the liver infection?
Hepatitis C is a viral infection that attacks the liver. Infection with hepatitis C can lead to serious liver disease, including cirrhosis and cancer. Hepatitis C virus (HCV) is transmitted by exposure to blood or other bodily fluids that contain HCV.
What is a direct acting antiviral?
of people who take them, depending on the type of HCV infection and treatment exposure. These new drugs are called direct-acting antivirals (DAAs). The U.S. Food and Drug Administration (FDA) approved the first of these medications for HCV treatment in 2011. Several more medications have been approved since that time.
Is generic medicine cheaper than brand name?
It also means there are no generic versions of these drugs yet. Generics are typically much cheaper than brand- name versions. The FDA determines how long this period of exclusivity will last. During this time, the pharmaceutical companies have a lot of freedom in establishing prices.
What are the criteria for liver disease?
These criteria may be based on: the severity of liver disease. whether the person avoids alcohol and drug use. whether the drug’s prescribed by a doctor who specializes in liver diseases. the life expectancy of the person seeking treatment. whether less expensive treatments could be used first.
Can hepatitis C be treated with drugs?
Today there are several drug options available that can cure hepatitis C infection — that’s the great news. What’s less great is the high cost of these drugs. However, there are many options you can explore to find help paying for these medications.
What is the cure rate for hepatitis C?
Direct-acting antivirals (DAAs) are associated with cure rates above 95% for hepatitis C virus (HCV). 1 However, the exorbitant costs of DAAs historically have made access prohibitive for many patients.
Why is Maryland not a direct acting agent for Medicare?
Objectives: Most Medicaid beneficiaries with hepatitis C virus (HCV) are not treated with direct-acting agents because of budget constraints, but they experience costly complications after becoming Medicare eligible. Maryland’s “total coverage” proposal could receive a credit from Medicare to offset Medicaid investments in treatments ...
What is the semi infectious disease model?
The semi-infectious disease model assessed the cost-effectiveness of HCV outcomes based on increased treatment probabilities under the total coverage scenario, compared with 2 scenarios reflecting the current payer model with standard coverage for all beneficiaries or prioritized coverage for all high-risk beneficiaries ( Figure 1 ). In the latter alternative, the 60% of patients with chronic HCV who had a liver fibrosis score of 2 or higher, as opposed to a fibrosis score of 0 or 1, received DAAs first, before lower-risk patients, in order to better manage budget impact. 15
Is DAA coverage for HCV?
Providing total coverage for DAA medications for all patients with HCV is systematically complex and may not be economically viable for state Medicaid programs that face some of the highest rates of HCV among payers. Joint Medicaid-Medicare coverage provides an efficient solution to treat all patients now to reduce harm caused by chronic infection in the United States. Recent price reductions for HCV treatments improve the outlook on affordability at the system level, as the $26,400-plus price tag still makes it inaccessible to individual Medicaid enrollees. Furthermore, the long-term costs of untreated HCV typically borne by Medicare are offset under this concept. The Maryland TCOC model gives Medicare the option of crediting Medicaid for spending money today that it will save on health care costs in the future. This is an approach to resolve the mismatch between investing today and getting future returns.
Is expanded coverage for hepatitis C cost effective?
Expanded coverage under a joint partnership by Medicare and Medicaid to treat all prevalent cases of hepatitis C virus (HCV) appears to be cost-effective by saving money and improving patient outcomes.
What percentage of people in prison have hepatitis C?
People who are incarcerated face an even tougher battle to get treatment for hepatitis C. Roughly 17 percent of prisoners are infected with hepatitis C, compared with about 1 percent of the general population. Prisons have a duty not to be deliberately indifferent to the medical needs of incarcerated people.
How much does Mavyret cost?
Insuring Your Health. In addition, Mavyret’s price tag of $26,400 for a course of treatment is significantly below that of other hepatitis C drugs whose sticker price ranges from about $55,000 to $95,000 to beat the disease.
How long does it take for mavyret to work?
The drug, Mavyret , is the first to be approved by the Food and Drug Administration that can cure all six genetic types of hepatitis C in about two months in patients who haven’t previously been treated. Other approved drugs generally require 12 weeks to treat the disease and often aren’t effective for all types of hepatitis C.
Does Delaware have Medicaid?
The Delaware resident was diagnosed with hepatitis C more than two years ago, but she doesn’t qualify yet for the Medicaid program’s criteria for treatment with a new class of highly effective but pricey drugs. The recent approval of a less expensive drug that generally cures hepatitis C in just eight weeks may make it easier for more insurers ...
How much did Medicaid increase in 2014?
In total, Medicaid spending on these 20 drugs with unit cost increases more than doubled from $146 million in 2014 to $486 million in 2015. Of the 20 drugs with the highest per-unit cost increases, nine were generics. Those products had price increases ranging from 140 percent to nearly 500 percent between 2014 and 2015.
How much does Tysabri cost?
Meanwhile, the Tysabri multiple sclerosis medicine sold by Biogen cost $39,767 per beneficiary and caused Part B to spend nearly $289 million. And the drug with the largest increase in unit cost was mitomycin, a generic chemotherapy treatment, which jumped 163 percent. There were six medicines for which unit costs increased more than 20 percent.
How many drugs are in Medicare Part D?
There were 40 drugs chosen from both Medicare Part D and Part B, and 70 drugs from Medicaid. The data does not include rebates, but some older rebate information for Medicare is provided. advertisement. There is a wealth of information, but here are some of the most interesting findings: Let’s start with Medicare Part D:
Who bought Daraprim?
At No. 2 was Daraprim, the life-saving anti-infective sold by Turing Pharmaceuticals. When the company was run by Martin Shkreli, Turing bought the drug and quickly jacked up the price by about 5,000 percent, causing a national sensation. Daraprim’s cost per unit rose 864 percent.
Shots
A 12-week regimen of Harvoni is 90 percent effective in curing an infection with hepatitis C, doctors say. It also costs about $95,000.
Treatments
A 12-week regimen of Harvoni is 90 percent effective in curing an infection with hepatitis C, doctors say. It also costs about $95,000.
